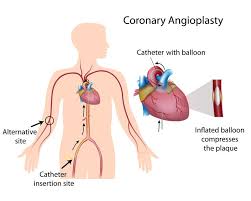
Coronary angioplasty is a non-surgical procedure that uses a balloon-tipped catheter to open narrowed or blocked coronary arteries, restoring blood flow to the heart. This process, also called percutaneous coronary intervention (PCI), often involves inserting a stent to keep the artery from closing again. It is used to treat coronary artery disease caused by atherosclerosis, where plaque buildup narrows the arteries.
What it is and how it works
- The problem: Atherosclerosis, or the buildup of plaque (fats, cholesterol, and other substances), can narrow or block the coronary arteries that supply blood to the heart.
- The procedure:
- A long, thin tube with a balloon on the tip (catheter) is guided through a blood vessel to the blocked coronary artery.
- A contrast dye is often used, and a special X-ray called a fluoroscopy allows the doctor to see the blockage.
- The balloon is inflated at the narrowed area, pressing the plaque against the artery walls to widen the vessel.
- The balloon is then deflated and removed, and the doctor checks that blood flow has improved.
Stent placement
- Purpose: A metal mesh tube called a stent is often placed during the procedure to help keep the artery open long-term.
- How it works: The stent is mounted on the balloon and expands as the balloon inflates. It is left inside the artery after the balloon is deflated and removed.
- Drug-eluting stents: These have medicine on them that helps prevent the artery from closing up again in the future.
When it’s done
- Can be performed emergently during a heart attack.
- Can also be done electively if a healthcare provider suspects heart disease.
Risks and recovery
- Risks: While generally safe, the procedure carries some risks, such as bleeding or bruising at the insertion site, allergic reaction to the dye, damage to the artery, or in rare cases, a heart attack or stroke.
- Recovery: The procedure is minimally invasive, and recovery time varies but is typically less than open-heart surgery

